Stem Cell Therapy
Stem cell therapy is a treatment method that uses stem cells to repair or regenerate damaged, diseased or dysfunctional tissues in the body.
Cerebellar Prolapse
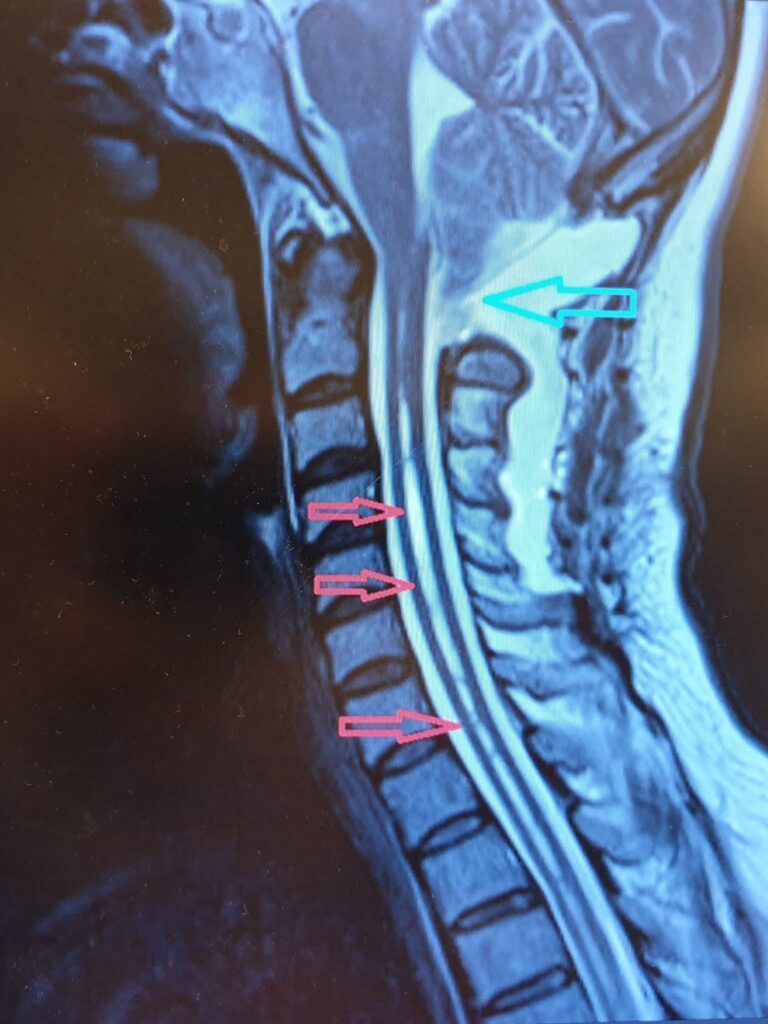
Cerebellar Prolapse Home Page / Cerebellar Prolapse (Chiari Malformation) What is Cerebellar Prolapse (Chiari Malformation) Chiari malformation (cerebellar prolapse) is a condition in which certain structures of the cerebellum, known as the center of balance, herniate into the spinal canal, compressing the brainstem. Signs and Symptoms Chiari malformation is usually discovered incidentally. In its advanced stages, it can cause headaches, balance disorders, clumsiness, dizziness, swallowing difficulties, and many other problems, particularly in children, triggered by straining, crying, or laughter. Headaches triggered by crying, straining, and laughter Balance disorders and clumsiness Dizziness Swallowing disorders Coordination problems Treatment Approaches While follow-up and rehabilitation are the primary treatment options in early cases, surgery is considered in advanced cases. Surgical procedures are performed to alleviate current symptoms or prevent future problems. 1. Conservative Treatment Regular follow-up and observation Physical therapy and rehabilitation Symptomatic treatment Lifestyle modifications 2. Surgical Treatment Surgical intervention may be necessary in advanced cases: Posterior fossa decompression Dura mater expansion Reducing pressure on the brainstem Treatment Goals The aim is to reduce current complaints, preserve neurological functions, and prevent future complications. RELATED DISEASES TMS (Transcranial Magnetic Stimulation) Tethered Cord Syndrome Spinal Fractures
TMS (Transcranial Magnetic Stimulation)
TMS (Transcranial Magnetic Stimulation) Home Page / TMS (Transcranial Magnetic Stimulation) What is Transcranial Magnetic Stimulation (TMS) or Brain Stimulation (TMS) treatment? The brain is an organ that functions through electrical impulses emitted by neurons. In some cases or diseases, electrical impulses in different parts of the brain may be disrupted. These disorders are treated externally through transcranial magnetic stimulation (TMS), or stimulation (TMS). What is the mechanism of action of TMS, and how is it applied? TMS is applied 2-3 cm above the skull using a coil. The magnetic field it creates activates an electrical current in the cerebral cortex, thereby depolarizing the neurons. TMS has different effects when applied at different frequencies: High-frequency TMS causes excitation (excitation) in the applied area, while low-frequency TMS causes inhibition (slowing). In repetitive TMS, the magnetic pulses arrive in a rapid series. The location, intensity, and time interval of stimulation are adjusted for various diseases. Where is TMS used? TMS can be used for many different psychiatric and neurological diseases. Psychiatric Diseases Major depression (FDA-approved) Anxiety disorders Hyperactivity and attention deficit disorder Neurological Diseases Migraine (FDA-approved) Parkinson's Essential tremor Tinnitus Other Areas of Use Obesity (suppressing the feeling of hunger) Treatment of depression during pregnancy A DRUG-FREE SOLUTION TO DEPRESSION IN PREGNANCY WITH TMS Depression can be observed in a portion of mothers, such as , during pregnancy and the early postpartum period. Treatment becomes particularly difficult because medications given for depression during pregnancy can be harmful to the baby. In addition to motivational interviews and cognitive behavioral studies, which are determined according to the severity of the mother's symptoms, TMS applied as a somatic treatment can help patients during pregnancy and the postpartum period. DOES IT HAVE ANY SIDE EFFECTS? Patients do not feel any pain during the TMS application. Current safety protocols adjust the amount of stimulation based on the individual's motor threshold. RELATED DISEASES: Tethered Cord Syndrome, Spinal Fractures, Carpal Tunnel Syndrome
Tethered Cord Syndrome
Tethered Cord Syndrome Home Page / Tethered Cord Syndrome This is the condition in which the spinal cord normally terminates below the L2 level of the spine due to the faster growth rate of the spinal bones than the spinal cord. Tethered cord syndrome (TSS) can occur in isolation or in association with conditions in which the spinal cord sac ruptures or becomes saccular (meningocele, meningomyelocele, lipomeningomyelocele, myeloschistocele, diastometomyelia, syringomyelia, and dermal sinusitis). Symptoms: Dermatological (SKIN) Findings: Hair growth, dimples, pitted redness, and holes on the skin of the waist may be signs of a tethered spinal cord. Orthopedic findings: Feet may turn inward, and legs may be bowed. Urological findings: Delayed urinary control or later-onset urinary incontinence may occur. Diagnosis and Treatment: Children with these conditions should definitely undergo an MRI, and if a tethered spinal cord is detected, spinal cord release should be performed. RELATED DISEASES: Spinal Fractures, Carpal Tunnel Syndrome, Piriformis Syndrome
Spinal Fractures
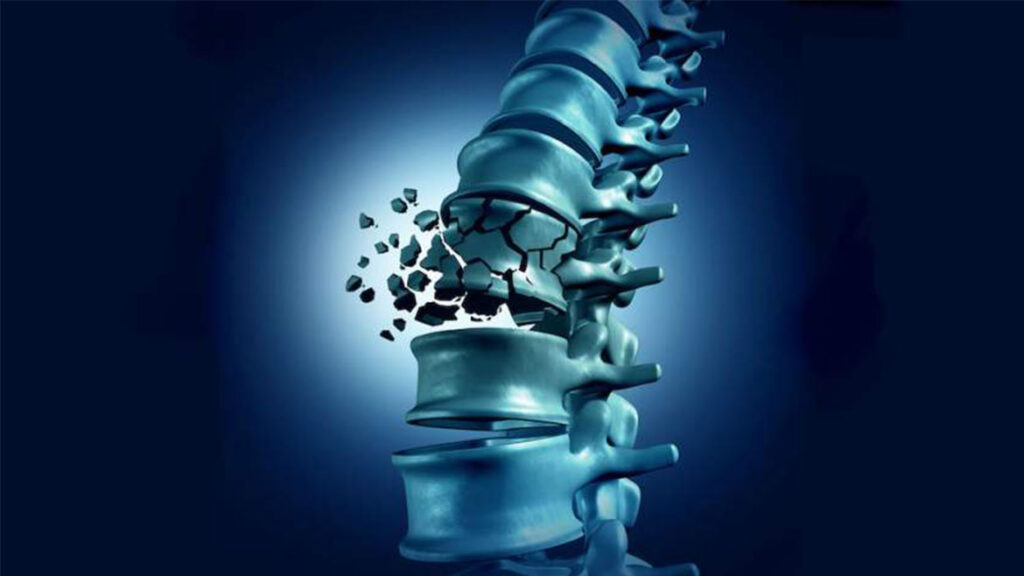
Spinal Fractures Home Page / Spinal Fractures Spinal fractures are one of the most common causes of severe back pain and backache, especially in older adults. Many patients who were previously prescribed bed rest for months for spinal fractures caused by falls or minor strains, including those with osteoporosis (osteoporosis), cancer patients, and those who suffered from spinal fractures due to falls or minor strains, can now be easily treated and experience rapid relief from severe pain. What is Vertebroplasty? Vertebroplasty is a specialized interventional treatment used to treat fractures of the anterior part of the spine, damage from cancer, or certain congenital vascular diseases. During the vertebroplasty procedure, a chemical called polymethylacrylate (bone cement) is injected into the damaged spinal bone under local anesthesia and radiological control, strengthening the bone. The patient is discharged the same day or the following day. RELATED DISEASES: Carpal Tunnel Syndrome, Piriformis Syndrome, Cervical Disc Herniation
Carpal Tunnel Syndrome
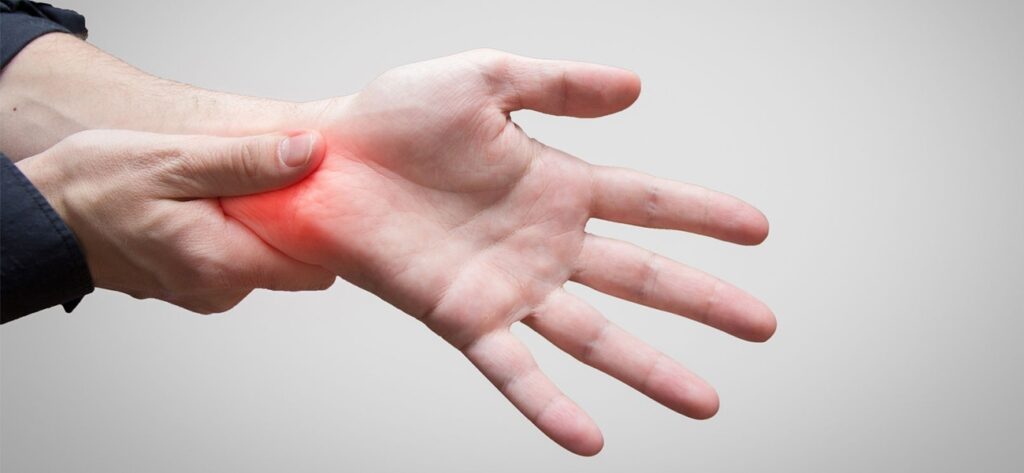
Carpal Tunnel Syndrome Home Page / Carpal Tunnel Syndrome Carpal Tunnel Syndrome (CTS) is a progressive condition affecting the first three fingers of one or both hands. It manifests as pain, numbness, and weakness due to compression of the median nerve, which is located in the middle of the wrist and distributes to the first three fingers. Causes of Carpal Tunnel Syndrome: Individuals with structurally narrow wrist canals are prone to developing clinical symptoms. It is more common in obese individuals, those who consume alcohol, those with diabetes, and those with vascular diseases. Carpal tunnel syndrome is caused by increased pressure within the canal. This pressure is related to the position of the hand. Mechanical factors in the workplace play a role in most cases. Frequent repetition of certain movements is associated with carpal tunnel syndrome. Risk Factors: Carpenters and manual laborers, tennis players, those who frequently wash dishes with their hands, drivers, those who engage in repetitive wrist movements, during pregnancy (temporary condition), symptoms of carpal tunnel syndrome. Patients often wake up a few hours after falling asleep with a feeling of swelling, numbness, and tingling throughout the entire hand. The fingers are stiff, and the patient feels swollen and tight; however, no objective change is actually observed. Patients shake and rub their hands, often getting out of bed, and relief occurs shortly thereafter. Sometimes, numbness recurs multiple times in a single night, causing severe sleep disturbances. Hand numbness awakening from sleep at night, a feeling of swelling and tension in the hand, finger stiffness, spread of numbness to the forearm, shoulder, and neck, and increased symptoms after housework. Loss of strength in the later stages, wasting of the palm muscles. Diagnosis of carpal tunnel syndrome: A definitive diagnosis can be made with an EMG test. Carpal Tunnel Syndrome Treatment: Conservative Treatment: In patients with severe sensory impairment and no motor impairment, nighttime rest wristbands that keep the wrist in a neutral position while allowing the fingers to move freely are very beneficial. Symptoms are relieved for a long time after hydrocortisone injection into the carpal tunnel. While low-dose oral cortisone therapy has been reported to yield good results, no further reports of the effects of this treatment have been provided. Surgical Treatment: Patients whose symptoms persist with medication should undergo surgery without further delay, meaning before nerve damage worsens. Relieving pressure on the nerve through surgery will prevent further damage. Surgical Features: No hospitalization required. Outpatient treatment is performed under local anesthesia. Pressure on the nerve is relieved. RELATED DISEASES: Piriformis Syndrome, Cervical Disc Herniation, Lumbar Disc Herniation
Piriformis Syndrome
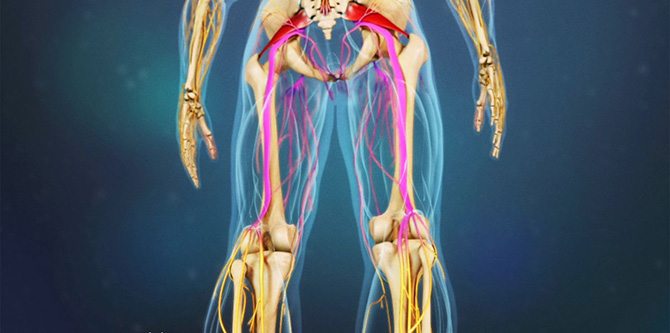
Piriformis Syndrome Home Page / Piriformis Syndrome Piriformis syndrome is a rare condition caused by the piriformis muscle in the buttocks pressing on the nearby sciatic nerve. It manifests as pain in the buttocks and legs. The piriformis is a flat muscle located in the buttocks. It originates in the lower spine and attaches to the upper surfaces of each thighbone, stabilizing the hip and enabling side-to-side movement of the hip, assisting in walking. A spasm in this muscle can compress the sciatic nerve, causing numbness, tingling, and pain in the buttocks, thighs, and legs on the side of the compressed sciatic nerve. Because it exhibits similar symptoms to certain conditions, such as a herniated disc, it can be confused with the patient. It can occur suddenly or develop gradually over time. It is six times more common in women than in men, because the quadriceps femoris muscle in the pelvis has a wider angle in women than in men. Types of Piriformis Syndrome Primary Piriformis Syndrome: It is related to the individual's anatomy. This is caused by the muscle and nerve structures varying from person to person. If the piriformis muscle is structurally incompatible with the nerve that passes directly beneath it, it is called primary piriformis syndrome. Secondary Piriformis Syndrome: It occurs due to muscle damage caused by trauma, lifestyle factors, and past illnesses. This type accounts for the majority of syndromes. Causes of Piriformis Syndrome Injuries: Traffic accidents, injuries that cause bleeding in the muscle, falls, sudden twisting of the hip, and trauma can cause piriformis damage. Lifestyle: The piriformis muscle can be damaged by excessive exercise, but it can also be damaged by prolonged inactivity. Inactivity, sitting for long periods, especially on hard surfaces, a shift in the center of gravity due to weight gain during pregnancy, excessive exercise, running, repetitive leg movements, and lifting heavy objects are among the causes. Anatomical Disorders: Leg length discrepancies, spinal curvature (scoliosis), previous hip surgery, a tumor in the hip area, or a ballooning of a blood vessel (aneurysm) can also cause piriformis damage. Piriformis Syndrome Symptoms: Pain that worsens with sitting, standing, or lying for more than 15-20 minutes; Numbness and tingling sensations radiating from the coccyx to the buttocks and back of the leg; Pain that improves with movement and increases with rest; Pain when rising from a sitting or squatting position; Weakness in the legs; Difficulty sitting; Difficulty walking, staggering; Pain when getting out of bed; Leg weakness due to muscle atrophy in later stages; In some cases, abdominal, hip, and groin pain; and in women, pain during intercourse. Piriformis Syndrome Treatment: Early, nonsurgical treatment is highly beneficial for piriformis syndrome. This method includes activities aimed at reducing muscle tension and spasms in daily life, hip strengthening exercises, physical therapy, and medication. Conservative Treatment: Activities aimed at reducing muscle tension, hip strengthening exercises, and physical therapy methods are applied. Injection Therapy: In some cases, injections may be administered to help reduce spasm and pain, relax the muscle, and reduce pressure on the sciatic nerve. Surgical Treatment: If this treatment fails, surgery should be considered as a last resort. Surgery reduces pressure on the sciatic nerve. RELATED DISEASES: Carpal Tunnel Syndrome, Cervical Disc Herniation, Lumbar Disc Herniation
Cervical Disc Herniation
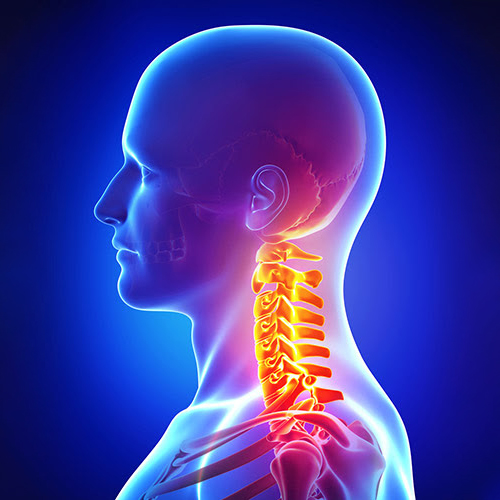
Cervical Disc Herniation Home Page / Cervical Disc Herniation (Cervical Disc Herniation) There are seven vertebrae in the neck. Between the vertebrae is a cartilage called a disc, which begins between the second and third vertebrae. The neck has the ability to move our head in all directions and supports the weight of the head. These movements are achieved through the discs and joints located between the vertebrae. The spinal cord passes through the cervical vertebrae. Nerves that control the movement of the arm muscles and provide sensation to the arms exit through the holes located between the vertebrae. The disc material consists of a relatively hard outer sheath between the two vertebrae and a gel-like soft tissue layer inside. When the outer sheath weakens or ruptures, the inner layer shifts outward and begins to press on the nerves. While the weakening or rupture of the outer layer more commonly causes neck pain, a cervical disc herniation, defined as the displacement of the inner layer outward, puts pressure on the nerve root, causing pain that radiates to the shoulder and arm. Arm pain, due to the pressure on the nerve roots, is often more severe than neck pain. Depending on the level of pressure on the nerve roots, arm and hand muscles may experience weakness and numbness. Which Patients Receive Surgery for Cervical Disc Herniation? Patients with persistent pain (severe pain radiating to the arm due to pressure on the nerve root). Patients who develop loss of strength due to pressure on the nerve root. Surgery involves removing the protruding disc between the vertebrae, relieving the nerves and spinal cord, and placing a disc prosthesis between the vertebrae to maintain movement. RELATED DISEASES: Stem Cell Therapy, Cerebellar Prolapse, TMS (Transcranial Magnetic Stimulation)
Herniated Disc
Herniated Disc Home Page / Herniated Disc What is a Herniated Disc? It is the rupture of the cartilage between the vertebrae in our lumbar region, compressing the nerves exiting the spinal cord. It first manifests as severe back pain, and later as pain radiating to the legs. Despite bed rest and treatment with some painkillers, surgical interventions are rapidly developing today for patients whose pain persists, whose social life is affected, and who experience paralysis in their feet. In cases where treatment is delayed, the pain and paralysis become permanent. Lumbar Anatomy The spine has three natural curvatures (curves) in the neck, back, and lumbar regions. Thanks to these curvatures, our spine minimizes the amount of load on it and can move flexibly. The lumbar region consists of 5 vertebrae and the sacrum (rump bone). The vertebrae stack on top of each other to form the spinal canal through which the spinal cord and nerves pass. The spine protects the spinal cord and nerves; The vertebrae allow our body movement. They are held together by cushions called "discs" at the front and "facet" joints at the back. Discs are essentially jelly-like shock absorbers that prevent the vertebrae from rubbing against each other. The function of the discs is to absorb the shocks that occur during walking, sitting, and lifting, and to evenly reduce the load on the vertebrae and distribute the weight evenly to the lower levels. The vertebrae are held together by two facet joints at the back. Each disc consists of two parts: a strong, fiber-woven outer section and a soft, jelly-like inner section. The strong outer section protects the soft, jelly-like inner section and enables flexible movement. In addition to these structures, the spine is supported by ligaments and muscles. Ligaments are strong bands that hold the discs and vertebrae in place. Muscles control movement, support the spine, and provide stability. The spinal cord is responsible for transmitting commands given by the brain to the other parts of the body. The spinal cord terminates in the upper lumbar region and gives nerve branches to the leg muscles, urinary bladder, and sexual organs. These nerves provide leg movement, sensation, urination, defecation, and sexual function. How Does a Herniated Disc Occur? In addition to many external factors, such as lifting a heavy load or performing an awkward movement, individual factors also play a significant role in the development of a herniated disc. Some people can lift 120 kg and experience no discomfort; others can lift 5 kg and develop a herniated disc. The most important individual factor is degeneration of the cartilage between the vertebrae, called the disc. Just as nothing in the universe is left to chance, the nutrition of the disc follows a specific plan and schedule. Certain substances pass through specific areas of the disc. However, as we age, the number of vessels supplying the disc decreases and they disappear completely after about age eight. After this age, the disc's nutrition is achieved through diffusion. The water content of the discs gradually decreases from childhood onward. While the water content in a fetal disc is 90, in children this ratio drops to 80 and in adults to 50-60. Consequently, the disc gradually shrinks and decreases in height. This is accompanied by nutritional deficiencies, microscopic changes, chemical changes, and degeneration caused by mechanical forces applied to the disc. The amount of oxygen and nutrients entering the disc gradually decreases, making it difficult to remove metabolic waste. The disc loses its elasticity over time and can no longer transmit force and distribute it evenly to surrounding tissues. The number of supporting cells within the disc, which play a role in repair, also decreases with age. Repair becomes impaired. When excessive pressure is placed on microfractures or when a person makes a wrong movement, the soft part of the disc can easily tear the surrounding capsule, protruding, and a herniated disc occurs. Once the groundwork is ready, the final straw is needed, which could be lifting a light object or simply coughing. Which Patients Should Undergo Surgery? If a patient treated with conservative, nonsurgical methods, despite all efforts, fails to improve—in other words, if they experience unbearable, persistent pain that naturally diminishes their quality of life—then they are a candidate for surgery. There's no need for them or those around them to endure constant suffering. Some patients improve with conservative treatment, but their condition recurs after a while. Sometimes they're in good shape, sometimes they're in bad shape. Some people experience this condition for years. With each relapse, their work, family, and social lives are severely impacted, virtually disrupted. These are often patients who are very afraid of surgery. Surgery is often considered for those whose herniated discs frequently recur, particularly those whose productivity and quality of work life are significantly reduced, disrupting their normal routine for weeks. The cause of their discomfort should be explained in detail to these patients, and the decision to undergo surgery should be left to them. Some patients also experience numbness, weakness, and weakening of their leg muscles, along with back and leg pain. They are constantly worsening. They must not be allowed to worsen further, and the necessity of surgery must be explained to them. Emergency Surgery: If a patient with a herniated disc experiences symptoms such as inability to urinate or defecate, numbness around the anus and genitals, or paralysis in the legs, they must undergo surgery immediately. In such a patient, even hours, even minutes, are crucial. Even in the middle of the night, surgery must be performed immediately to relieve pressure on the nerves. The idea that a herniated disc will heal on its own if left to wait is not true for every patient. Our long-standing experience has shown that successful surgery shortens the recovery period, and patients generally return to work sooner. RELATED DISEASES: Scoliosis, Spinal Canal Narrowing, Lumbar Disc
Scoliosis
Spinal Cord Tumors Home Page / Scoliosis (Curvature of the Spine) Scoliosis is a sideways curvature of the spine that can be seen in the thoracic or lumbar regions. In a normal and healthy spine, the vertebrae form a straight line from top to bottom when viewed from behind, namely in the neck, back, and lumbar regions. In scoliosis, the vertebrae shift to the right or left and also rotate around their own axes. While the curvature can be noticed even when standing upright when viewed from behind, it is sometimes less obvious and can only be detected when bending forward, during checkups, and on x-rays. How is it detected? Scoliosis is most often seen in adolescence, and if not treated early, it can cause irreparable damage to both the cosmetic and the cardiovascular and respiratory systems. It is important for the patient to observe their own body shape and recognize certain symptoms in order to diagnose the disease. These symptoms are; Shoulder disparity Asymmetry in the lumbar region A protrusion of one side of the spine A bony prominence on one side of the back (shoulder blade appearance) A shift in body balance to the right or left Diagnostic Methods Scoliosis is diagnosed by a standing X-ray of the entire spine and the presence of one or more of the above-mentioned symptoms during a clinical examination. When a scoliosis diagnosis is made, an MRI examination is necessary to determine the cause. On standing anteroposterior and lateral radiographs of the entire spine, the angle between the vertebrae where the curve begins and ends is measured, and the progression of this angle is monitored. This angle is called the Cobb angle. Surgery is the only option for curves greater than 40 degrees and for patients with continuing growth potential. Surgery can be successfully performed with implants (screw-rods) placed in the back and lumbar region. Neuromonitoring Monitoring spinal cord functions during surgery (neuromonitoring) is a method that increases the reliability of the procedure for both the patient and the physician and is routinely used at our center. RELATED DISEASES: Narrowing of the Spinal Canal, Lumbar Spondylolisthesis, Hydrocephalus
